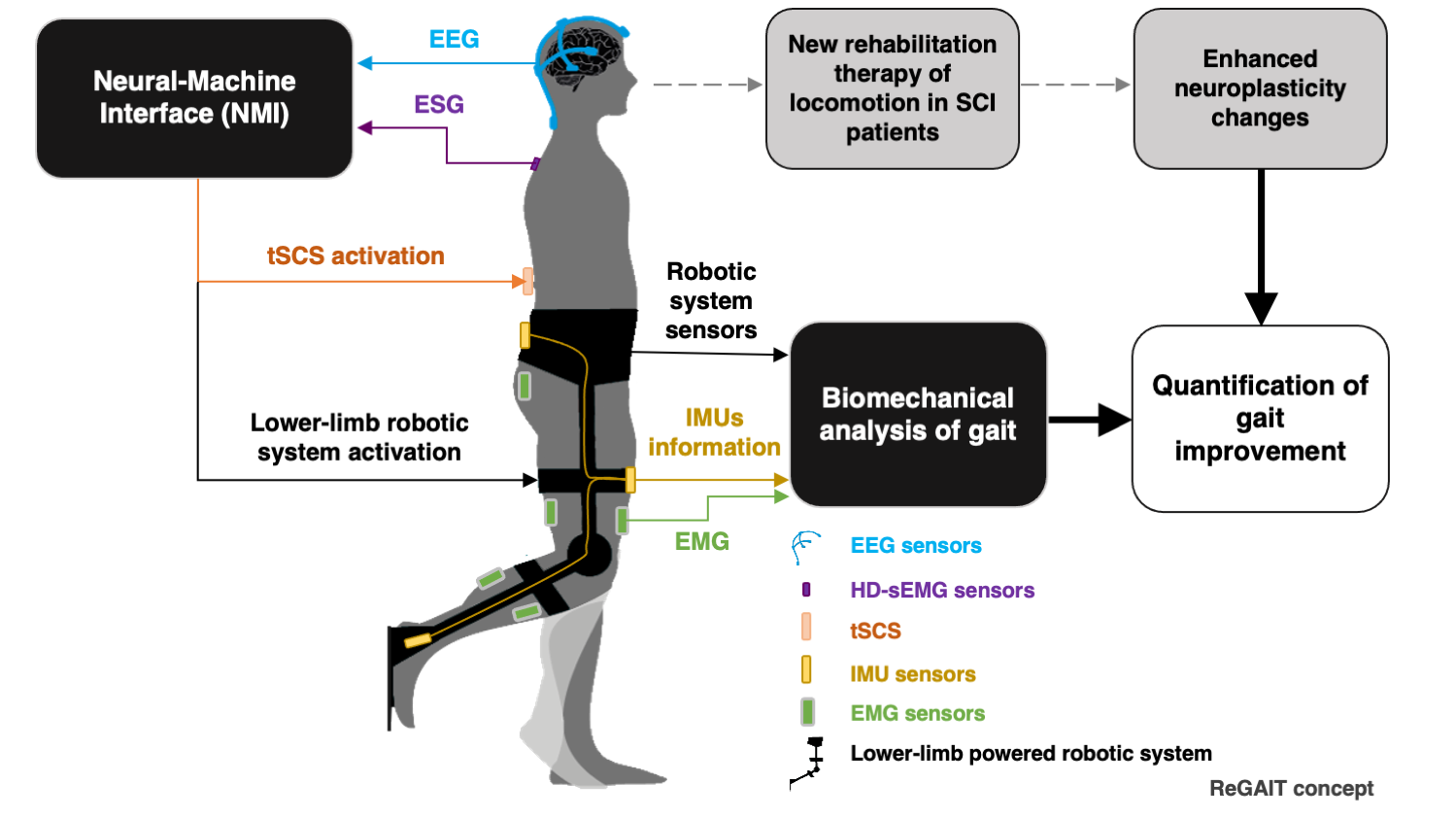
ReGAIT: A new rehabilitation approach of locomotion for incomplete spinal cord injury patients by integrating neural interfaces, lower-limb powered robotic systems and transcutaneous spinal current stimulation strategies
SUBPROJECT 1: Development of a self-tuned Neural-Machine Interface for closed-loop control of lower-limb exoskeletons (PID2021-124111OB-C31)
- Principal Investigators: José M. Azorín & Eduardo Iáñez
- Center: Miguel Hernández University of Elche, Spain
SUBPROJECT 2: Design of transcutaneous spinal current stimulation strategies for rehabilitation of gait (PID2021-124111OB-C32)
- Principal Investigators: Hatice Kumru
- Center: Guttmann Institute, Spain
SUBPROJECT 3: Development of a novel strategy to analyze the effect on gait biomechanics when combining lower-limb powered exoskeletons controlled by Neural-Machine Interfaces and transcutaneous spinal current stimulation in incomplete spinal cord injured patients (PID2021-124111OB-C33)
- Principal Investigators: Angel M. Gil-Agudo & Mónica Alcobendas Maestro
- Center: Hospital for Paraplegics, Spain
Journals, Conferences, Data repositories and protocols
Tesis, Dissemination activities, Project Activities & Events
Abstract
Spinal Cord Injury (SCI) is one of the major motor disorders due to damage in the human nervous system leading to physical impairment in Western society. These conditions will in general disrupt sensory and motor pathways that in turn lead to permanent pathological gait, resulting in impaired independent ambulation. Subsequent restoration of motor function is often variable and incomplete. Usually, therapists try to recover some residual ability for movement when possible, acting over the distal physical level, trying to influence the neural system through mechanisms of neural plasticity (BOTTOM-UP approach). Traditional therapies to improve functional ambulation for patients in the sub-acute phase (3-11 weeks post-injury) use overground training and require designed preparatory exercises, observation by a physical therapist, direct manipulation of the limbs during gait over a regular surface, followed by supervised walking. This kind of physical rehabilitation is both physically burdensome and time-consuming for the therapists. With recent advances in robotic technologies, lower-limb robotic exoskeletons have emerged as aids for over-ground, bipedal ambulation for individuals with motor limitations. However, there have been many discussions over the clinical relevance of exoskeletons, being still elusive the specific benefits of long-term use of exoskeletons in gait training.
This project proposes a new approach to produce enhanced neuroplasticity changes during rehabilitation of locomotion in incomplete thoracic SCI patients by associating and synchronizing the use of lower-limb powered robotic systems with neural activity voluntarily generated by patients and with stimulation of the spinal cord. The neural activity will be detected by means of a Neural-Machine Interface (NMI) composed by a Brain-Machine Interface (BMI) based on electroencephalography (EEG) and a Spinal cord Machine Interface (SMI) based on electrospinography (ESG). On the other hand, different transcutaneous spinal current stimulation (tSCS) strategies for rehabilitation of gait will be explored to induce neuroplasticity, selecting the most effective to be synchronized with the lower-limb exoskeleton commanded by the NMI. Thus, the project will combine a TOP-DOWN rehabilitation approach, i.e. association of neural activity voluntarily generated by the patient with the afferent feedback provided by an exoskeleton, and a BOTTOM-UP approach based on transcutaneous spinal current stimulation. It is expected that this new rehabilitation intervention improves brain plasticity, which is believed to be the responsible for functional improvements. To evaluate the performance progress of the gait rehabilitation, new metrics will be defined based on biomechanical analysis techniques. These metrics will allow us to have an objective knowledge of the gait and of the biomechanical and physiological mechanisms of the recovery achieved. The new rehabilitation approach will be evaluated with incomplete SCI patients in two hospitals focused on research and clinical therapies in SCI people: National Hospital for Paraplegics (HNP: Hospital Nacional de Parapléjicos, Toledo, Spain) and Guttmann Institute (IG: Institut Guttmann, Barcelona, Spain), which are members of the consortium of this project.
Journals:
- Gracia, D. I., Iáñez, E., Ortiz, M., & Azorín, J. M. (2026). Denoising Non-Invasive Electroespinography Signals by Different Cardiac Artifact Removal Algorithms. Biosensors, 16(2), 82. https://doi.org/10.3390/bios16020082
- Soriano-Segura, P., Ortiz, M., Polo-Hortigüela, C. Iáñez, E. & Azorín. J.M. (2025). Characterization of error-related potentials during the command of a lower-limb exoskeleton based on deep learning. J NeuroEngineering Rehabil 23, 11 (2026). https://doi.org/10.1186/s12984-025-01833-3
- Polo-Hortigüela, C., Ortiz, M., Soriano-Segura, P., Iáñez, E., & Azorín, J. M. (2025). Time-Frequency Analysis of Motor Imagery During Plantar and Dorsal Flexion Movements Using a Low-Cost Ankle Exoskeleton. Sensors, 25(10), 2987. https://doi.org/10.3390/s25102987
- Hernandez-Navarro, A., Ros-Alsina, A., Yurtseven, M., Wright, M., Kumru, H. (2025) Non-invasive cerebral and spinal cord stimulation for motor and gait recovery in incomplete spinal cord injury: systematic review and meta-analysis. J NeuroEngineering Rehabil 22, 53 (2025). https://doi.org/10.1186/s12984-025-01557-4
- Soriano-Segura, P., Ortiz, M., Iáñez, E., & Azorín, J. M. (2024). Design of a brain-machine interface for reducing false activations of a lower-limb exoskeleton based on error related potential. Computer Methods and Programs in Biomedicine, 255, 108332. https://doi.org/10.1016/j.cmpb.2024.108332
- Herrera-Valenzuela D, Sinovas-Alonso I, de-los-Reyes-Guzmán A, Gil-Agudo A, del-Ama AJ. Improvement of the gait deviation index for spinal cord injury to broaden its applicability: the reduced gait deviation index for spinal cord injury (rSCI-GDI). Front Bioeng Biotechnol. 2024;12. https://doi.org/10.3389/fbioe.2024.1431596
- Blanco-Coloma L, García-González L, Sinovas-Alonso I, Torio-Álvarez S, Martos-Hernández P, González-Expósito S, Gil-Agudo A, Herrera-Valenzuela D. Validation of inertial measurement units based on waveform similarity assessment against a photogrammetry system for gait kinematic analysis. Front Bioeng Biotechnol. 2024;12. https://doi.org/10.3389/fbioe.2024.1449698
- Ferrero, L., Soriano-Segura, P., Navarro, J., Jones, O., Ortiz, M., Iáñez, E., Azorín, J.M., Contreras-Vidal, J.L. (2024). Brain–machine interface based on deep learning to control asynchronously a lower-limb robotic exoskeleton: a case-of-study. Journal of NeuroEngineering and Rehabilitation, 21(1), 48. https://doi.org/10.1186/s12984-024-01342-9
- Hatice Kumru; Aina Ros-Alsina; Loreto García Alén; Joan Vidal; Yury Gerasimenko; Agusti Hernandez; Mark Wrigth (2024) International Journal of Molecular Sciences, IP. 5.6: » Improvement in Motor and Walking Capacity During Multisegmental Transcutaneous Spinal Stimulation in Individuals with Incomplete Spinal Cord Injury. International Journal of Molecular Sciences 2024-04-19. https://doi.org/10.3390/ijms25084480
- Juan, J. V., Martínez, R., Iáñez, E., Ortiz, M., Tornero, J., & Azorín, J. M. (2024). Exploring EEG-based motor imagery decoding: a dual approach using spatial features and spectro-spatial Deep Learning model IFNet. Frontiers in Neuroinformatics, 18, 1345425. https://doi.org/10.3389/fninf.2024.1345425
- Sinovas-Alonso I, Herrera-Valenzuela D, de-los-Reyes-Guzmán A, Cano-de-la-Cuerda R, del-Ama AJ, Gil-Agudo Á. Construct Validity of the Gait Deviation Index for People With Incomplete Spinal Cord Injury (GDI-SCI). Neurorehabil Neural Repair. 2023;37(10):705-715. https://doi.org/10.1177/15459683231206747
- Ferrero, L., Quiles, V., Ortiz, M., Iáñez, E., Gil-Agudo, Á., & Azorín, J. M. (2023). Brain-computer interface enhanced by virtual reality training for controlling a lower limb exoskeleton. Iscience, 26(5). https://doi.org/10.1016/j.isci.2023.106675
- Kumru H, García-Alén L, Ros-Alsina A, Albu S, Valles M, Vidal J. (2023) Transcutaneous Spinal Cord Stimulation Improves Respiratory Muscle Strength and Function in Subjects with Cervical Spinal Cord Injury: Original Research. Biomedicines. 2023;11(8):2121. Published 2023 Jul 27. https://doi.org/10.3390/biomedicines11082121
- Kumru H, Castillo-Escario Y, Jane R, Vidal J, García-Alén L. (2023) Effect of Transcutaneous Cervical Spinal Cord Stimulation on Trunk Function in Subjects with Cervical Spinal Cord Injury. J Spine Res Surg. 2023;5(4). Published 2023 December. https://doi.org/10.26502/fjsrs0067
International and national conferences:
- IEEE Systems, Man, and Cybernetics (SMC 2025): Bhambhani, Y., Ortiz, M., Polo-Hortigüela, C., Quiles, V., Carlo Cavaliere-Ballesta, Eduardo Iáñez, & José M. Azorín. (2025). Supervised and Semi – Supervised Machine Learning Networks applied for control of a Lower – Limb Exoskeleton. Proceedings of the 2025 IEEE International Conference on Systems, Man, and Cybernetics (SMC). Viena, Austria.
- Juan, J. V., Pacheco, S., Iáñez, E., Ortiz, M., Tornero, J., & Azorín, J. M. (2025). Improving Motor Imagery Decoding Through EEG Frequency Band Analysis. Proceedings of the 2025 IEEE International Conference on Metrology for eXtended Reality, Artificial Intelligence and Neural Engineering (MetroXRAINE) (p. 1107). Ancona, Italia.
- Polo-Hortigüela, C., Quiles, V., Soriano-Segura, P., Cavaliere-Ballesta, C., Bhambhani, Y., Ortiz, M., Iáñez, E., & Azorín, J. M. (2025). Asynchronous Control of an Exoskeleton with BMI: Evaluation and Validation of EEG Processing and Classification Strategies for Motor Imagery. Proceedings of the 2025 IEEE International Conference on Metrology for eXtended Reality, Artificial Intelligence and Neural Engineering (MetroXRAINE) (pp. 1290-1295). Ancona, Italia.
- «Quiles, V., Polo, C., Soriano-Segura, P., Ortiz, M., Iáñez, E., & Azorín, J. M. (2025). Design of an Asynchronous BMI with Interpretable Neural Networks
for Exoskeleton Control: A Proof of Concept on Data Evolution and Scalability Over One Week. Proceedings of the 2025 47th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC). Copenhague, Dinamarca. ISBN: 979-8-3315-8618-8.» - IEEE Engineering in Medicine and Biology Society (EMBC 2025): Soriano-Segura, P., et al. (2025). [Título del artículo de Paula en EMBC 2025]. Proceedings of the 2025 47th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC). Copenhague, Dinamarca. ISBN: 979-8-3315-8618-8.
- Soriano-Segura, P., García-Villalón, J., Ortiz, M., Iáñez, E., Bayón-Calatayud, M., & Azorín, J. M. (2024, November). Comparing Generic and Personalized Models for Detecting Error Potentials During Gait Initiation of a Lower-Limb Exoskeleton. In International Conference on NeuroRehabilitation (ICNR 2024), Converging Clinical and Engineering Research on Neurorehabilitation V – Volume II, pp. 680-683. November 5-8, 2024, La Granja de San Ildefonso, Spain
- Juan, J.V., Martínez, R., Iáñez, E., Ortiz, M., Tornero, J., Azorín, J.M. (2025, February). Mitigating Catastrophic Forgetting in Pedaling Motor Imagery Decodification Using Continuous Progressive Neural Network. In International Conference on NeuroRehabilitation (ICNR 2024), Converging Clinical and Engineering Research on Neurorehabilitation V – Volume I, pp. 89-93. November 5-8, 2024, La Granja de San Ildefonso, Spain
- Gracia, D. I., Polo-Hortigüela, C., Iáñez, E., Ortiz, M., & Azorín, J. M. (2024, November). A Novel Technique for Removing Electrocardiography Artifacts from Electroespinography Signals by Preserving Low Frequencies. In International Conference on NeuroRehabilitation (ICNR 2024), Converging Clinical and Engineering Research on Neurorehabilitation V – Volume II, pp. 698-702. November 5-8, 2024, La Granja de San Ildefonso, Spain
- Polo-Hortigüela, C., Gracia, D. I., Quiles, V., Ortiz, M., Iáñez, E., & Azorín, J. M. (2024, November). Design and Construction of a Low-Cost Ankle Exoskeleton for Neurorehabilitation System. In International Conference on NeuroRehabilitation (ICNR 2024), Converging Clinical and Engineering Research on Neurorehabilitation V – Volume II, pp. 703-707. November 5-8, 2024, La Granja de San Ildefonso, Spain
- C. Polo-Hortigüela, J.V. Juan, M. Ortiz, E. Iáñez, J.M. Azorín. (2024). Análisis de señales EEG en movimientos de flexión plantar y dorsal mediante el empleo de un exoesqueleto de bajo coste parala caracterización de la acción motora. Congreso anual de la sociedad española de ingeniería biomédica (CASEIB 2024), pp: 381-384, November 13- 15, 2024, Sevilla, Spain.
- D. I. Gracia, J. A. Flores-Yepes, J. M. Cano, Ortiz, M., & J. M. Azorín. (2024). Optimización de parámetros para el filtrado de artefactos cardíacos en señales electroespinográficas no invasivas: un caso de estudio. Congreso anual de la sociedad española de ingeniería biomédica (CASEIB 2024), pp: 201-204, November 13- 15, 2024, Sevilla, Spain.
- Gracia, D. I., Polo-Hortigüela, C., Iáñez, E., Ortiz, M., & Azorín, J. M. (2024, November). A Novel Technique for Removing Electrocardiography Artifacts from Electroespinography Signals by Preserving Low Frequencies. In International Conference on NeuroRehabilitation (ICNR 2024), Converging Clinical and Engineering Research on Neurorehabilitation V – Volume II, pp. 698-702. November 5-8, 2024, La Granja de San Ildefonso, Spain
- Polo-Hortigüela, C., Gracia, D. I., Quiles, V., Ortiz, M., Iáñez, E., & Azorín, J. M. (2024, November). Design and Construction of a Low-Cost Ankle Exoskeleton for Neurorehabilitation System. In International Conference on NeuroRehabilitation (ICNR 2024), Converging Clinical and Engineering Research on Neurorehabilitation V – Volume II, pp. 703-707. November 5-8, 2024, La Granja de San Ildefonso, Spain
- Soriano-Segura, P., García-Villalón, J., Ortiz, M., Iáñez, E., Bayón-Calatayud, M., & Azorín, J. M. (2024, November). Comparing Generic and Personalized Models for Detecting Error Potentials During Gait Initiation of a Lower-Limb Exoskeleton. In International Conference on NeuroRehabilitation (ICNR 2024), Converging Clinical and Engineering Research on Neurorehabilitation V – Volume II, pp. 680-683. November 5-8, 2024, La Granja de San Ildefonso, Spain
- García-Villalón, J., Soriano-Segura, P., Ortiz, M., Iáñez, E., Azorín, J. M. (2024, November). Decoding motor imagery of starting walk with a lower-limb exoskeleton by using EEGnet and TSNE. Neuroscience 2024. October 5-9, 2024, Chicago, EEUU.
- Gracia, D. I., Polo-Hortigüela, C., Bayón-Calatayud, M., Iáñez, E., Ortiz, M., & Azorín, J. M. (2024, October). A Case Study for Removing Cardiac Artifacts from Non-Invasive Electrospinography Signals. In 2024 IEEE International Conference on Metrology for eXtended Reality, Artificial Intelligence and Neural Engineering (MetroXRAINE), pp. 1147-1152. October 21-23, 2024, St. Albans, London, UK.
- Polo-Hortigüela, C., Gracia, D. I., Soriano-Segura, P., Ortiz, M., Iáñez, E., Cavaliere-Ballesta, C., & Azorín, J. M. (2024, October). Motor Imagery Analysis of EEG Signals Using a Low-Cost Ankle Exoskeleton. In 2024 IEEE International Conference on Metrology for eXtended Reality, Artificial Intelligence and Neural Engineering (MetroXRAINE), pp. 1135-1140. October 21-23, 2024, St. Albans, London, UK.
- Sempere, J.M., Gracia, D.I., Azorín, J.M., Úbeda, A., Iáñez, E. (2024, September). Optimización del registro en tiempo real de sensor de fuerza. XLV Jornadas de Automática, September 4-6, 2024. Málaga, Spain
- Soriano-Segura, P., García-Villalón, J., Ortiz, M., Martínez, E. I., & Azorín, J. M. (2024). Protocolo para detectar el ErrP durante la marcha con exoesqueleto. XLV Jornadas de Automática, September 4-6, 2024. Málaga, Spain
- Villalón, J. G., García, M. O., Segura, P. S., Martínez, E. I., & Poveda, J. M. A. (2024). Análisis de la influencia de EEGNET en una BMI basada en máquina de estados para el control de un exoesqueleto de miembro inferior. In Actas del Simposio de Robótica, Bioingeniería y Visión por Computador, pp. 185-190, May 29-31 2024, Badajoz, Spain
- Laura Ferrero,Soriano Segura, P.,Jacobo Navarro,Oscar Jones,Ortiz Garcia, M.,Iañez E,Azorín, J.M.,José Contreras-Vidal (2023, November). Optimizing Motor Imagery Training for Lower-Limb Exoskeleton Control Through BCI. In Proceedings of XII Congreso Iberoamericano de Tecnologías de Apoyo a la Discapacidad (IBERDISCAP 2023), pp: 232-237, November 20-22, 2023, Sao Paulo, Brasil.
- Soriano Segura, P.,Laura Ferrero,Ortiz Garcia, M.,Iañez E,Azorín, J.M. (2023, November). Protocol for evaluating error related potentials in a lower-limb exoskeleton commanded by a brain-machine interface. In Proceedings of XII Congreso Iberoamericano de Tecnologías de Apoyo a la Discapacidad (IBERDISCAP 2023). IBERDISCAP 2023, pp: 232-237, November 20-22, 2023, Sao Paulo, Brasil.
- P. Soriano-Segura, L. Ferrero, D. I. Gracia, M. Ortiz, E. Iáñez and J. M. Azorín, «Analysis of Different Stimulus for Evoking the ErrP Potential in a MI-BMI for Starting the Gait with a Lower-Limb Exoskeleton,» 2023 IEEE International Conference on Systems, Man, and Cybernetics (SMC), Honolulu, Oahu, HI, USA, 2023, pp. 3653-3658, doi: 10.1109/SMC53992.2023.10393944.
- Soriano-Segura, P., Ferrero, L., Gracia, D. I., Ortiz, M., Iáñez, E., & Azorín, J. M. (2023, October). Analysis of Different Stimulus for Evoking the ErrP Potential in a MI-BMI for Starting the Gait with a Lower-Limb Exoskeleton. In 2023 IEEE International Conference on Systems, Man, and Cybernetics (SMC), pp. 1124-1128. October 1-4, 2023, Oahu, Hawaii.
- Soriano-Segura, P., Gracia, D.I, Ferrero, L., Iáñez, E., Ortiz, M., Azorín, J.M. (2023). Study of the variability of single trial error potential in relation to P300 and N500. XLIV Jornadas de Automática, 116-120. https://doi.org/10.17979/spudc.9788497498609.116
- L. Ferrero et al., «Transfer Learning with CNN Models for Brain-Machine Interfaces to command lower-limb exoskeletons: A Solution for Limited Data,» 2023 45th Annual International Conference of the IEEE Engineering in Medicine & Biology Society (EMBC), Sydney, Australia, 2023, pp. 1-4, doi: 10.1109/EMBC40787.2023.10340008.
- P. Soriano-Segura, L. Ferrero, M. Ortiz, E. Iáñez and J. M. Azorín, «Analysis of Error Potentials generated by a lower limb exoskeleton feedback in a BMI for gait control,» 2023 45th Annual International Conference of the IEEE Engineering in Medicine & Biology Society (EMBC), Sydney, Australia, 2023, pp. 1-4, doi: 10.1109/EMBC40787.2023.10340275.
- Hatice Kumru, Aina Ros Alsina, M. Wright, Loreto Garcia, Joan Vidal. «N°50 – To Improve Gait Function during Multilevel Transcutaneous Spinal Cord Stimulation Following Incomplete Motor Spinal Cord Injury». Clinical Neurophysiology, vol. 150, junio de 2023, pp. e87-88. https://doi.org/10.1016/j.clinph.2023.03.059.
- Hatice Kumru. Improving Transcutaneous Spinal Cord Stimulation paradigms in health and/or tSCS for the recovery of different motor function following spinal cord injury individuals. Institut Guttmann (Barcelona, Spain). 45th Annual International Conference of the IEEE Engineering in Medicine and Biology Society, 24-27 julio 2023, Sydney (Australia). Invited speaker.
- Hatice Kumru, Yolanda Castillo, Loreto García-Alen, Eloy Opisso Neurofisiología en Neurorehabilitación. 3ª Jornada científica sobre electrodiagnóstico neurológico (SELECNE), 6 marzo 2024
- Hatice Kumru. “Nuevos campos de la Neurofisiología Clínica y técnicas en desarrollo”. LX Reunión Anual de la Sociedad Española de Neurofisiología Clínica (SENFC), 3 octubre 2024, Barcelona (Spain). Session moderator.
- Agustín Hernández y Hatice Kumru. Póster en ICNR 2024: “Changes in spasticity and medullar reflexes after tSCS application”. ICNR 2024, 5 noviembre 2024, Segovia (Spain).
- Hatice Kumru. “Transcutaneous spinal cord stimulation (scTS) en lesión medular”. XXXIV Congreso de la Sociedad Valenciana de Medicina Física y Rehabilitación (SVMEFR), 1 marzo 2025, Valencia (Spain).
- Hatice Kumru «Advancing neurorehabilitation: new frontiers in spinal cord injury and stroke treatments, cellular therapy, andneuromodulation”. International Congres son Neurorehabilitation and Neural Repair, 15 mayo 2025, Maastricht (Netherland). Symposium moderationw with James Guest, José Pones and Xabier Urra.
- Hatice Kumru. “Structure and connextivity informed stimulation of the nervous system: how the micro level may guide macro level stimulation interventions”. Reunión conjunta de la Red Española de Estimulación Cerebral y de la Asociación Española de Estimulación Cerebral. Jornadas de estimulación cerebral 2025: Brain stimulation meeting 2025: where are we going? 26 mayo 2025, Sevilla (Spain). Session moderator with Guillermo Sánchez-Garrido, Miguel Ángel García-Cabezas, Lorena Chanes and Juha Silvanto.
- Hatice Kumru. “Restoring Function After SCI: The Emerging Potential of Transcutaneous SC” in the session “From Research to Reality: Advances in Spinal Cord Stimulation for Improved Outcomes”. Reunión conjunta de la Red Española de Estimulación Cerebral y de la Asociación Española de Estimulación Cerebral. Jornadas de estimulación cerebral 2025: Brain stimulation meeting 2025: where are we going? 26 mayo 2025, Sevilla (Spain).
- Hatice Kumru. “Avances en el tratamiento del dolor neuropático: el papel de la neuromodulación y neuroestimulación”. Congreso Nacional de Paraplejia, 12 de junio 2025, A Coruña (Spain).
Data repositories and protocols:
- Error Related Potential at the start of the gait with a lower limb exoskeleton (UMH-Zenodo). https://doi.org/10.5281/zenodo.10828804
- Synchronously recorded gait kinematic data with Inertial Measurement Units and a photogrammetry system for a validation assessment (HNP-Zenodo). https://doi.org/10.5281/zenodo.11242602
- Error Related Potential in motion to stop the gait with a lower limb exoskeleton (UMH-Zenodo). https://doi.org/10.5281/zenodo.14190392
- EEG Signal Dataset During Dorsiflexion and Plantar Flexion Movements (UMH-Zenodo). https://doi.org/10.5281/zenodo.14672334
- An ESG Database of Spinal Cord Activity During Gait-Related Tasks and Motor Imagery Exercises (UMH-Zenodo). https://doi.org/10.5281/zenodo.14615203
- Development of a Novel Strategy to Analyze the Effect on Gait Using Transcutaneous Spinal Current Stimulation in Incomplete Spinal Cord Injured Patients (IG – NCT07289191 – clinicaltrials.gov). https://clinicaltrials.gov/study/NCT07289191
Tesis:
- Laura Ferrero Montes. Interfaz cerebro-máquina multiparadigma para el control de la marcha con un exoesqueleto de miembro inferior. Directores: José María Azorín Poveda, Mario Ortiz García. Universidad Miguel Hernández de Elche. Fecha de lectura: 13/02/2024. Calificación: Sobresaliente “Cum Laude” por unanimidad
- Patricio Eduardo Barría Aburto. Nuevas aproximaciones para la rehabilitación de pacientes con Accidente Cerebrovascular (ACV) mediante estimulación eléctrica funcional y exoesqueletos robóticos: Medición de efectos biomecánicos y clínicos. Director: José María Azorín Poveda. Universidad Miguel Hernández de Elche. Fecha de lectura: 18/09/2023. Calificación: Sobresaliente “Cum Laude” por unanimidad
- Vicente Quiles Zamora. Diseño, implementación y entrenamiento de interfaces cerebro-máquina basadas en eventos de la marcha para control de exoesqueletos. Director: José María Azorín Poveda, Eduardo Iáñez Martínez. Universidad Miguel Hernández de Elche. Fecha de lectura: 22/05/2025. Calificación: Sobresaliente “Cum Laude” por unanimidad
- Javier Vicente Juan Poveda. Sistema de neurorrehabilitación de miembro inferior basado en interfaz cerebro-máquina y pedalina. Directores: José María Azorín Poveda, Eduardo Iáñez Martínez y Jesús Tornero López. Universidad Miguel Hernández de Elche. Tesis con mención industrial en realización. Fecha de defensa estimada: 2026.
- Paula Soriano Segura. Desarrollo de interfaces cerebro-máquina auto-corregibles para el control de la marcha de exoesqueletos de miembro inferior. Directores: José María Azorín Poveda, Mario Ortiz García. Universidad Miguel Hernández de Elche. Tesis en realización. Fecha de defensa estimada: 2026.
- Desirée Irene Gracia Laso. Exploración del uso de ESG para el desarrollo de interfaces neurales. Directores: José María Azorín Poveda, Eduardo Iáñez Martínez. Universidad Miguel Hernández de Elche. Tesis en realización. Fecha de defensa estimada: 2026.
- Cristina Polo Hortigüela. Diseño y desarrollo de un sistema de neurorrehabilitación basado en un exoesqueleto de bajo coste y una interfaz cerebro-máquina. Directores: Mario Ortiz García, Eduardo Iáñez Martínez. Universidad Miguel Hernández de Elche. Tesis en realización. Fecha de defensa estimada: 2026.
Dissemination activities:
| Demonstration of the ReGAIT project at Hospital for Paraplegics in Toledo, June 1st 2026 |
| ReGait is a research coordinated project by the Universitas Miguel Hernández (UMH), the National Hospital for Paraplegics in Toledo, and the Institut Guttmann, aiming to improve rehabilitation for individuals with incomplete spinal cord injury using advanced technologies. The project combines non-invasive neural interfaces (electroencephalography and electrospinography) to record nervous system signals and control exoskeletons that assist the patient’s gait; transcutaneous spinal cord stimulation (tSCS) to modulate spinal circuits related to movement; and motion and electromyography sensors to record biomechanical parameters and precisely analyze clinical progress. |
 |
 |
 |
 |
| Several media outlets have covered the presentation of the project |
| media. |
 |
| more details… |
| 5th International congres on Neurorehabilitation and Neural Repair, Maastricht, Netherlands – 2025 (Hatice Kumru) | LXXVII Reunión Anual SEN (Sociedad Española de Neurología), Sevilla, Spain – 2025 (Hatice Kumru) |
 |
 |
| XXVII Jornadas Técnicas del Institut Guttmann, Badalona, Spain – 2025 (José M. Azorín, Hatice Kumru) | Brain Stimulation Conference 2025, Sevilla, Spain – 2025 (Hatice Kumru) |
 |
 |
| Congreso de Medicina Física Valenciana, Valencia, Spain – 2025 (Hatice Kumru) | Annual meeting ISCoS – 2025 (Hatice Kumru) |
 |
 |
| European Congress of Clinical Neurophysiology (ECCN), London – 2025 (Hatice Kumru) | |
 |
Project Activities & Events:
| ReGAIT meeting at Hospital for Paraplegics in 2024 | ReGAIT meeting at Miguel Hernández University of Elche in 2024 |
 |
 |
| ReGAIT meeting at Guttmann Institut in 2024 | ReGAIT meeting at Hospital for Paraplegics in 2023 |
 |
 |
| Experiments with patients while using Lokomat | Experiments using H3 exoskeleton |
 |