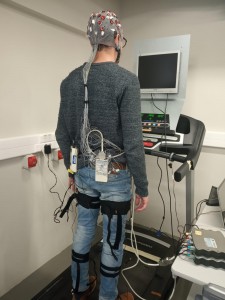
Controlling lower-limb exoskeletons by means of brain-machine interfaces to assist people with walking disabilities
Stroke and Spinal Cord Injury (SCI) are two of the major motor disorders due to damage in the human nervous system leading to physical impairment in Western society. These conditions will in general disrupt sensory and motor pathways that in turn lead to permanent pathological gait, resulting in impaired independent ambulation. Walking incorrectly creates a stigma and makes patients more susceptible to injury, affecting quality of life. Ambulation after trauma has long been a research topic, but more progress is needed.
With recent advances in robotic technologies, lower-limb robotic exoskeletons have emerged as aids for over-ground, bipedal ambulation for individuals with motor limitations. Interfaces between robotic exoskeletons and users are often implemented via a combination of mechanical and electrical devices. However, these interfaces are not what humans naturally use. The usability and clinical relevance of these robotics systems could be further enhanced by brain-machine interfaces (BMIs). BMIs bypass motor systems of any kind. BMIs make context-based decisions from recordings of the users brain activity, thus allowing direct and voluntary operation of the devices beyond users diminished physical capabilities. Although the feasibility of using BMIs to control lower-limb exoskeletons has been demonstrated, important challenges have to be still addressed to deploy these systems as assistive devices in the clinic and at home: (1) Robust BMIs with better performances have to be developed to send safely basic commands (walk and stop) to exoskeletons; (2) BMIs for turning left/right exoskeletons, increasing/decreasing their speed, or stopping them if unexpected obstacles appear have to be implemented for providing more capabilities to these systems; (3) Training schemes to reduce the number of training sessions required to use BMIs, and to reach higher performances have to be developed; and (4) More clinical studies have to be carried out to validate the health benefits of using these systems. All these challenges will be addressed in the WALK project.
The WALK project will go beyond the current state-of-the-art by developing more robust BMIs with higher performances not only able to control the exoskeletons for walking and stopping safely, but also to send them commands for turning left/right, increasing/decreasing their speed, or stopping them if unexpected obstacles appear. To improve the performance of the new BMIs and reduce the number of training sessions, new training strategies based on transcranial direct current stimulation (tDCS) and virtual reality will be developed. Furthermore, the project will demonstrate how the use lower-limb exoskeletons commanded by BMIs could have health benefits for SCI people, particularly with respect to pain, spasticity and autonomic activity.
Thus, the WALK project will allow people with locomotion difficulties to command lower-limb robotic exoskeletons by means of BMIs in order to provide them walking assistance in the clinic and at home. This will contribute that neurologically injured patients have higher activity at home and participation in society.